COVID-19
What is Corona Virus?
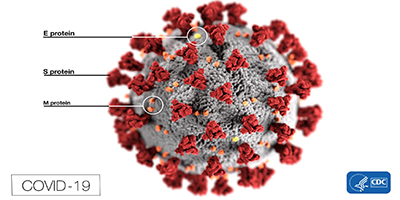
Corona viruses are a large family of viruses which may cause illness in animals or humans. In humans, several coronaviruses are known to cause respiratory infections ranging from the common cold to more severe diseases such as Middle East Respiratory Syndrome (MERS) and Severe Acute Respiratory Syndrome (SARS). The most recently discovered coronavirus causes coronavirus disease COVID-19.
What is COVID-19?
COVID-19 is the infectious disease caused by the most recently discovered corona virus. This new virus and disease were unknown before the outbreak began in Wuhan, China, in December 2019.
How is COVID-19 spread?
The virus that causes COVID-19 mainly spreads from person to person. This usually happens when an infected person coughs, sneezes, or talks near other people. The virus can be passed easily between people who live together. But it can also spread at gatherings where people are talking close together, shaking hands, hugging, sharing food, or even singing together.
Doctors also think it is possible to get sick if you touch a surface that has the virus on it and then touch your mouth, nose, or eyes. A person can be infected and spread the virus to others even without having any symptoms. This is why keeping people apart is one of the best ways to slow the spread.
It is also possible for the virus to spread from an infected person to an animal, like a pet, but this seems to be uncommon. There is no evidence that a person could get the virus from a pet.
There is also no evidence that COVID-19 can be spread through the water in a pool or hot tub. However, because the virus can spread when people are close together, activities like swimming in a crowded pool are still risky.
Experts do not think the virus is spread through food like some other viruses.
What are the symptoms of COVID-19? Can COVID-19 be prevented?
Symptoms usually start 4 or 5 days after a person is infected with the virus. But in some people, it can take up to 2 weeks for symptoms to appear. Some people never show symptoms at all.
Most people (about 80%) recover from the disease without needing special treatment. People with fever, cough, and difficulty breathing should seek medical attention.
Common symptoms include:
- Fever
- Cough
- Trouble breathing
- Feeling tired
- Shaking chills
- Muscle aches
- Headache
- Sore throat
- Problems with sense of smell or taste
Some people have digestive problems such as nausea or diarrhoea. There have also been reports of rashes or other skin symptoms. For example, some people with COVID-19 develop reddish-purple spots on their fingers or toes.
For most people, symptoms improve within a few weeks. However, some people continue to have symptoms for weeks or months. Doctors are still learning about the long-term effects of COVID-19.
Am I at risk for getting seriously ill?
Around 1 out of every 6 people who gets COVID-19 becomes seriously ill and develops difficulty breathing.
Older people and those with underlying medical problems such as serious heart disease, chronic kidney disease, type 2 diabetes, chronic obstructive pulmonary disease (COPD), sickle cell disease, or obesity are at higher risk.
People who have a weak immune system for other reasons (for example, HIV infection or certain medicines), asthma, cystic fibrosis, type 1 diabetes, or high blood pressure may also be at higher risk for serious illness.
What should I do if I have symptoms?
If you have a fever, cough, trouble breathing, or other symptoms of COVID-19, call your doctor. If your symptoms are not severe, it is best to call before you go in. Many people with only mild symptoms should stay home and avoid contact with others until they recover.
If you need to visit a clinic or hospital, wear a mask covering your nose and mouth to help protect others.
Healthcare staff may ask you to wait in an area away from other people to maintain social distancing.
If you are severely ill and need immediate medical attention, try to call ahead if possible. This allows healthcare providers to take precautions to protect others. If you believe you are having a medical emergency, call for an ambulance (in India, dial 108).
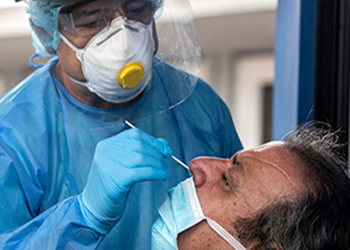
Is there a test for the virus that causes COVID-19?
Yes. If your doctor suspects you have COVID-19, they may take a swab from inside your nose and/or throat for testing. If you are coughing up mucus, a sample of the mucus may also be tested. These tests help determine whether you have COVID-19 or another illness.
There is also a blood test that can show whether a person has had COVID-19 in the past. This is called an antibody test.
Antibody tests are generally not used to diagnose active COVID-19 infection or to make treatment decisions. However, they are useful for understanding how many people in a community were infected without knowing it and for studying whether reinfection is possible.
Testing strategy for COVID-19: Click Here
How is COVID-19 treated?
Many people can stay home while they recover. However, people with serious symptoms or other health problems may need hospitalization.
Doctors are studying several possible treatments for COVID-19. In some cases, doctors may recommend medicines that appear to help certain patients who are severely ill. Participation in a clinical trial may also be advised. A clinical trial is a scientific study that tests new medications to determine their effectiveness.
Updated clinical management protocol for COVID-19 (Dated: 03 July 2020): Click Here
Guidelines for home isolation: Click Here
What can I do to cope with stress and anxiety?
It is normal to feel anxious or worried about COVID-19. Feeling stressed or lonely is also common, especially when daily routines are disrupted or when you cannot meet friends and relatives.
Most people do not become seriously ill from COVID-19. Being informed, prepared, and taking steps to reduce your risk can help you feel more in control. Focus on reliable information, practice healthy habits, and try not to panic.
Which are different investigational therapies?
At present, the use of these therapies is based on limited available evidence. As the situation evolves and more data become available, recommendations may be updated. The use of these drugs is also subject to limited availability in the country. Currently, these drugs should only be used in a defined subgroup of patients.
i. Remdesivir (Under Emergency Use Authorization)
Remdesivir may be considered in patients with moderate disease (those requiring oxygen), provided none of the following contraindications are present:
- AST/ALT greater than 5 times the upper limit of normal (ULN)
- Severe renal impairment (eGFR < 30 ml/min/m² or need for hemodialysis)
- Pregnancy or lactation
- Children below 12 years of age
Dose: 200 mg IV on day 1, followed by 100 mg IV daily for 4 days (total duration: 5 days).
ii. Convalescent Plasma (Off Label)
Convalescent plasma may be considered in patients with moderate disease who are not improving (despite steroid therapy) and whose oxygen requirements are progressively increasing.
Special prerequisites include:
- ABO compatibility and cross-matching of donor plasma
- Neutralizing antibody titre above the recommended threshold (if unavailable, plasma IgG titre against S-protein RBD > 1:640)
- Close monitoring of the recipient for several hours post-transfusion
- Avoid use in patients with IgA deficiency or immunoglobulin allergy
Dose: Variable (4–13 ml/kg), usually 200 ml as a single dose infused slowly over not less than 2 hours.
This document will be updated as more evidence becomes available. These therapies represent potential off-label or investigational use of medications based on expert consensus and available evidence. Informed and shared decision-making is essential before prescribing.
iii. Tocilizumab (Off Label)
Tocilizumab may be considered in patients with moderate disease and progressively increasing oxygen requirements, as well as in mechanically ventilated patients not improving despite steroid use. Long-term safety data in COVID-19 remains largely unknown.
Special considerations before use include:
- Presence of elevated inflammatory markers (CRP, Ferritin, IL-6)
- Close monitoring for secondary infections and neutropenia
- Contraindicated in PLHIV, active systemic bacterial or fungal infections, tuberculosis, active hepatitis, ANC < 2000/mm³, or platelet count < 100,000/mm³
Dose: 8 mg/kg (maximum 800 mg) diluted in 100 ml normal saline, administered IV over 1 hour. The dose may be repeated once after 12–24 hours if required.
Dr. Sagar Raiya's Publications
See Our all publications and presentations
