Home oxygen therapy Long-term supplemental oxygen therapy
Purpose of this blog:
There are many patients taking home oxygen, sometimes self-prescribed or by family physician. This blog will help to make patients and doctors aware regarding indications of home oxygen therapy. Inadequate usage (flow or hours/day) or excess usage (higher flow rates) can cause side effects like any other medicines.
Long-term oxygen therapy (LTOT) increases survival and improves the quality of life of hypoxemic patients with chronic obstructive pulmonary disease (COPD) and is often prescribed for other patients with hypoxemic chronic lung disease
Continuous LTOT is needed for following patients with chronic lung diseases.
- 1. Arterial oxygen tension (PaO2) less than or equal to 55 mmHg (7.32 kPa), or a pulse oxygen saturation (SpO2) less than or equal to 88 percent
- 2. PaO2 less than or equal to 59 mmHg (7.85 kPa), or an SpO2 less than or equal to 89 percent, if there is evidence of
a. Cor pulmonale,
b. Right heart failure, or
c. Erythrocytosis (hematocrit >55 percent)
Some patients require oxygen during sleep
For patients with normal awake oxygenation, oxygen may be prescribed during sleep if any of the following occur during sleep:
- the PaO2 is 55 mmHg or less,
- the SpO2 is 88 percent or less,
- the PaO2 decreases more than 10 mmHg and/or
- the SpO2 decreases more than 5 percent
Some patients require oxygen during sleep
Special consideration:
Air travel —
Patients with a resting room air pulse oxygen saturation (SpO2) <92 percent at sea level are candidates for supplemental oxygen during air travel.
Patients with a resting room air SpO2 between 92 and 95 percent at sea level need further assessment to determine the need for oxygen in-flight.
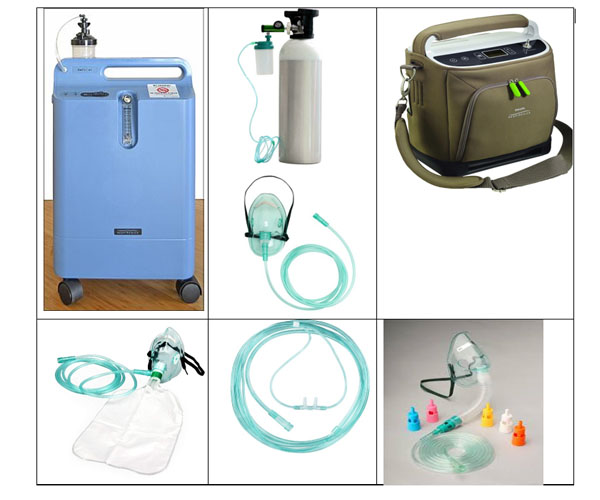
Oxygen sources and interfaces:
Oxygen cylinder, concentrators (including small portable devices).
Oxygen canula, oxygen mask, non-rebreather mask, venturi mask.

Dr. Sagar Raiya's Publications
See Our all publications and presentations
