Latent Tuberculosis Infection (LTBI)
Purpose of this blog
To make the general public and general/family physicians aware of this entity so as to avoid unnecessary testing for LTBI and treatment with anti-TB drugs.
What is Latent Tuberculosis Infection?
Latent tuberculosis infection (LTBI) is defined as a state of persistent immune response to stimulation by Mycobacterium tuberculosis antigens with no evidence of clinically manifest active TB.
In simple terms, Latent tuberculosis infection (LTBI) is the presence of Mycobacterium tuberculosis in the body without signs and symptoms, or radiographic or bacteriologic evidence of tuberculosis (TB) disease.
Is there a test for latent TB infection?
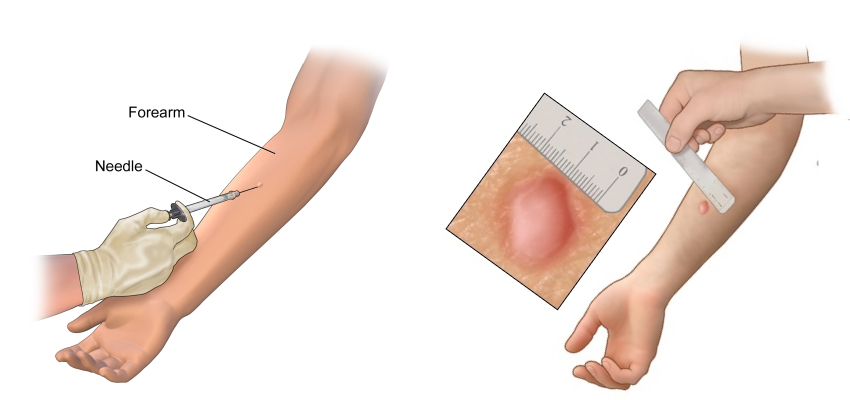
Tuberculin skin test (Mantoux test) and Interferon gamma release assay (IGRA – TB Gold / QuantiFERON).
However, one must know that there is no gold standard test for LTBI. Also, TST / IGRA are not used as diagnostic tests for active tuberculosis disease.
What is recommendation for testing and treating people LTBI? World health organization and Indian recommendations.
India, with one-fourth of the global burden of TB, has nearly 40 percent of the population infected with Mycobacterium tuberculosis.
Treating 40 percent of the population for LTBI based on Tuberculin Skin Test (TST) positivity or Interferon Gamma Release Assay is neither rational nor practicable; hence, a focused approach is needed.
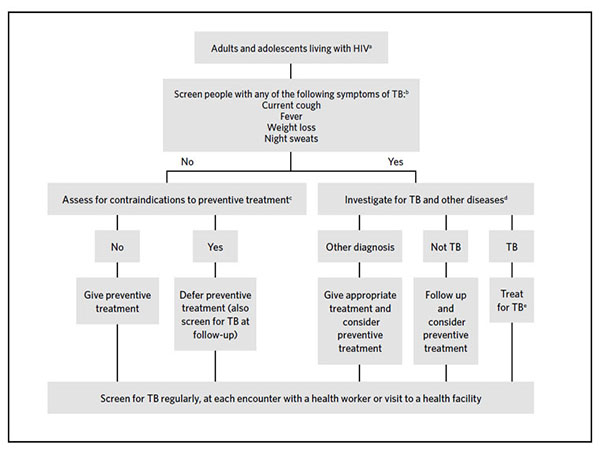
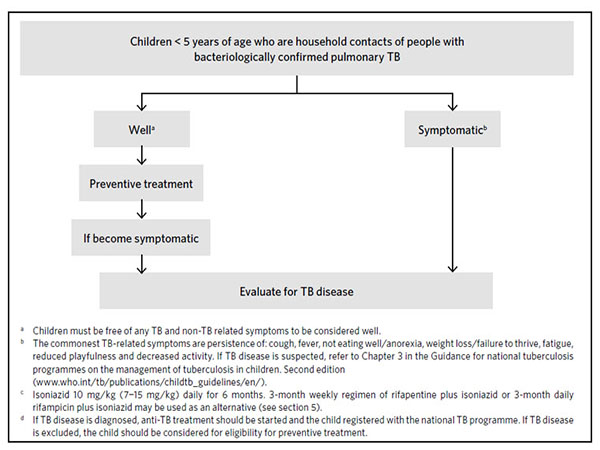
World health organization recommends screening in following population.
- Adults, adolescents, children, and infants living with HIV
- HIV-negative children aged < 5 years (< 6 years in India) who are household contacts of people with bacteriologically confirmed pulmonary TB
-
Other HIV-negative at-risk groups (as per WHO, not included in Indian guidelines yet):
- Patients initiating anti-TNF treatment, patients receiving dialysis, patients preparing for organ or hematological transplant, and patients with silicosis (receiving long-term corticosteroids – included in NTEP)
- In low TB incidence countries: prisoners, health workers, immigrants from high TB burden countries, homeless people, and people who use illicit drugs
- Systematic testing is NOT recommended for people with diabetes, harmful alcohol use, tobacco smokers, or underweight people unless included above
In India, as per National Tuberculosis Elimination Programme
People living with HIV and children less than 6 years need not be checked by TST or IGRA for latent TB. Treatment can be initiated after excluding active TB disease.
Isoniazid treatment for 6 months is required.
Studies have demonstrated that Isoniazid (INH) taken for at least 6 months in persons with LTBI reduced subsequent TB incidence by 25 to 92 percent, with differences largely explained by treatment completion.
In clinical situations, the most obvious group for LTBI treatment includes high-risk patients such as those receiving long-term corticosteroids, immunosuppressants, HIV-infected individuals, and juvenile contacts of sputum-positive index cases.
Differentiating between Latent TB Infection and TB Disease
| Latent TB Infection | TB Disease |
|---|---|
| No symptoms or physical findings suggestive of TB disease | Symptoms may include fever, cough, chest pain, weight loss, night sweats, hemoptysis, fatigue, and decreased appetite |
| TST or IGRA result usually positive | TST or IGRA result usually positive |
| Chest radiograph is typically normal | Chest radiograph is usually abnormal (may be normal in advanced immunosuppression or extrapulmonary disease) |
| Respiratory specimens, if done, are smear and culture negative | Respiratory specimens are usually smear or culture positive |
| Cannot spread TB bacteria to others | May spread TB bacteria to others |
| Should consider treatment for LTBI to prevent TB disease | Needs treatment for TB disease |
Dr. Sagar Raiya's Publications
See Our all publications and presentations
